This wide range is likely due to the various pericarditis etiologies studied and researcher variation in the definition of what constituted a supraventricular arrhythmia. Though data related to the incidence of arrhythmias in the setting of pericarditis are sparse, atrial fibrillation appears to be the most common across studies occurring at rates ranging from 4.3% to 25%. AFL occurs in similar clinical causes as atrial fibrillation, including but not limited to pericarditis. In one population-based investigation of AFL, among 58,820 patients in central Wisconsin, those at highest risk for developing AFL were patients with heart failure and chronic obstructive pulmonary disease, with the arrhythmia being uncommon in structurally normal hearts.

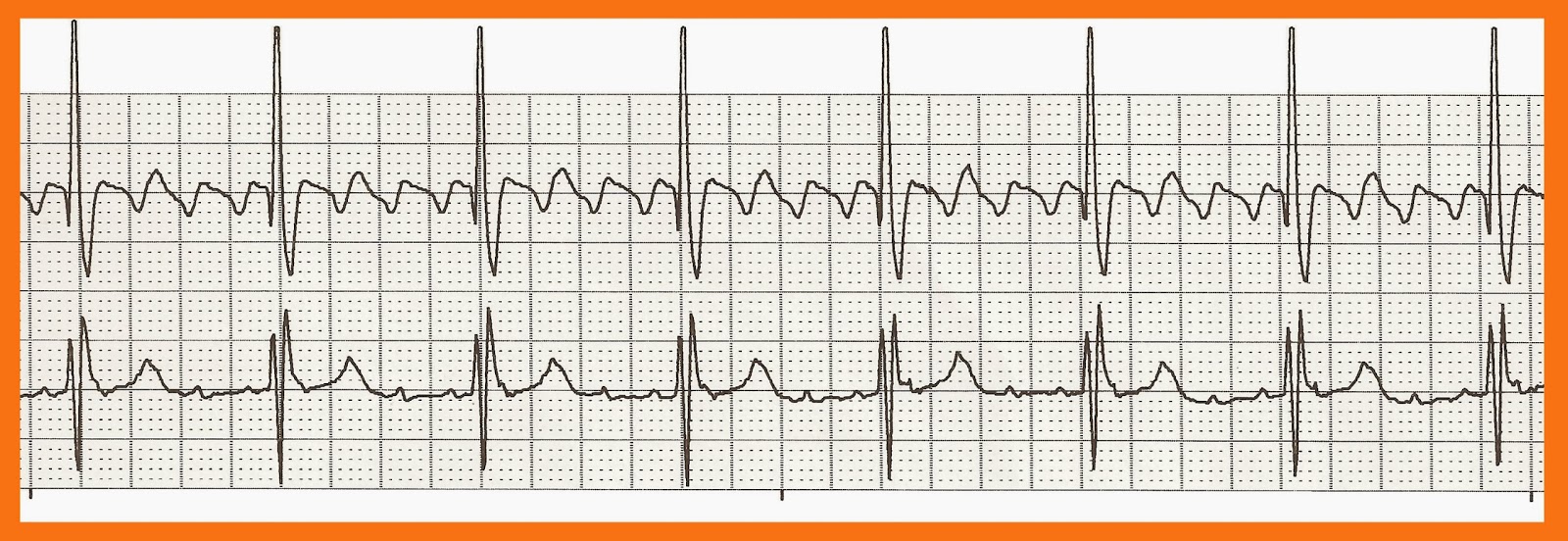
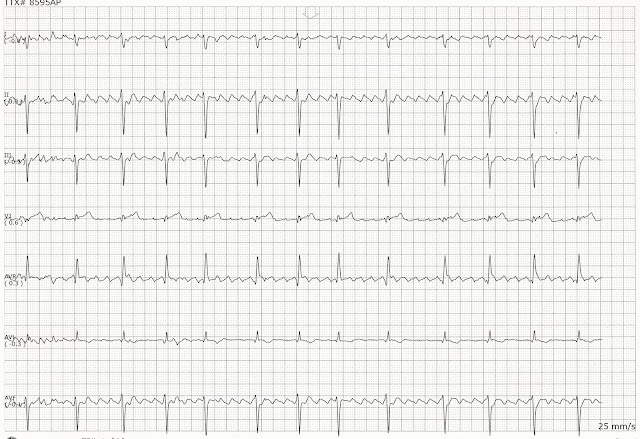
A typical atrial activity has been highlighted in Figure 1, and the ECG in Figure 2 highlights the atrial activity in the patient. Short-acting intravenous diltiazem was restarted and up-titrated for adequate rate control with hemodynamic stability.Īdenosine was subsequently administered and revealed AFL with variable AV block. He received an amiodarone load intravenously for rhythm control and renally dosed apixaban for a CHA₂DS₂-VASc score of five. The patient initially received boluses of intravenous diltiazem and transitioned briefly to a continuous diltiazem infusion, which was discontinued due to hypotension.
A trans-thoracic echocardiogram showed a preserved ejection fraction of 55-60% with moderate concentric hypertrophy without pericardial effusion. C-reactive protein, fibrinogen, and brain natriuretic peptide (BNP) were all elevated at 8.3 mg/dL, 583 mg/dl, 182 pg/mL, respectively. Thyroid-stimulating hormone was within normal limits at 1.902 lU/ml. Coronavirus 2019 (COVID-19) nasal rapid PCR was negative. Influenza A, B, and respiratory syncytial virus (RSV) nasal polymerase chain reaction (PCR) were negative. Troponin-I was within normal limits at 0.01 ng/mL. Labs were negative for electrolyte abnormalities and creatinine was 1.5 mg/dL (baseline 1.5-1.9 mg/dL). The initial ECG was significant for supraventricular tachycardia interpreted as new-onset atrial fibrillation with a rapid ventricular response. Case PresentationĪn 83 year-old-male with hypertension, stage three chronic kidney disease, hypothyroidism, transient ischemic attack, and sleep apnea presented with three weeks of pleuritic chest pain, fatigue, subjective fevers, and progressive shortness of breath. ECG findings post-cardioversion in normal sinus rhythm were consistent with pericarditis, which was likely the cause for his new-onset AFL. After a failed attempt at rate control, the patient underwent cardioversion. We present a case of an 83-year-old-man with supraventricular tachycardia determined to be AFL status post an adenosine trial. A pericardial friction rub may be heard during auscultation. On ECG, there may be widespread concave ST elevations and PR depressions with reciprocity in aVR. Presentation varies depending on the underlying etiology but often includes chest pain characterized as sharp, pleuritic, and improved by leaning forward. It is characterized by pericardial sac inflammation due to numerous causes such as infectious, neoplastic, inflammatory, autoimmune, metabolic, pharmacologic, or toxic.
Pericarditis is a known trigger for cardiac arrhythmias. AFL is uncommon in structurally normal hearts and can be seen in clinical contexts similar to those presenting with atrial fibrillation. Clinical presentation is often dependent on the ventricular rate and can lead to dyspnea, fatigue, palpations, and lightheadedness. Atypical flutter occurs outside the CTI around areas of atrial scar tissue. On electrocardiogram (ECG), typical p-waves are absent, and the atrial activity is seen in a sawtooth pattern known as “F waves” in leads II, III, and aVF. Typical flutter is defined by a macro-reentrant circuit around the cavotricuspid isthmus (CTI), generally in a counterclockwise rotation. Atrial flutter (AFL) is an arrhythmia characterized by rapid, regular, atrial depolarizations at a characteristic rate of between 250 and 350 beats per minute with a 2:1 relation between atrial and ventricular activity.

